Mycosis Fungoides Overview: Signs and Available Treatments
Mycosis fungoides is a slow-growing form of cutaneous T-cell lymphoma that often starts with patchy, scaly areas that can be mistaken for eczema or psoriasis. This overview explains how the rash commonly appears, what early staging like stage 1A typically indicates, and how clinicians confirm the diagnosis with skin biopsies and supportive blood testing such as flow cytometry. It also reviews treatment approaches ranging from topical medications and phototherapy to radiation and systemic options used when disease is more persistent or advanced.
Mycosis fungoides can be easy to miss at first because it often looks like everyday irritation. This overview walks through the most common signs of this rare skin lymphoma, why it can mimic other conditions, and the treatment options doctors commonly use to control symptoms and slow progression.
What Mycosis Fungoides Is
Mycosis fungoides is the most common form of cutaneous T-cell lymphoma (CTCL), a cancer of certain immune cells that primarily shows up in the skin. It often develops slowly over years, which is one reason people may cycle through multiple creams and diagnoses before CTCL is considered.
Because early disease can resemble dermatitis, a frequent question is what does skin eczema look like compared with something more serious. Eczema commonly causes itchy, inflamed patches that can ooze or crust, and it often improves with moisturizers and topical steroids. Mycosis fungoides may itch too, but it can persist despite typical eczema care and may recur in the same areas.
Common Signs: How The Rash Can Look And Feel
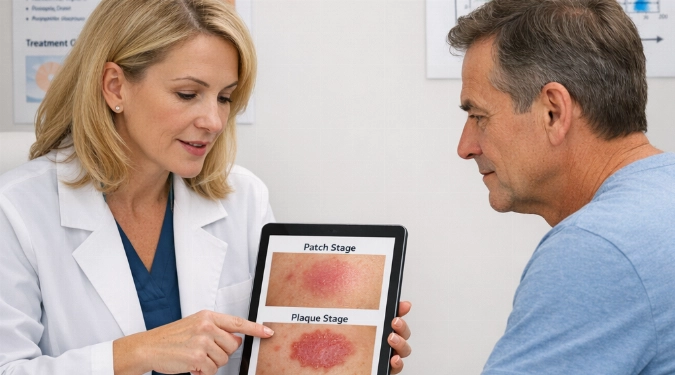
Early mycosis fungoides may appear as flat, scaly patches, sometimes with uneven color (pink, red-brown, or lighter than surrounding skin). Over time, some people develop thicker plaques, and in more advanced cases, tumors can form. This is why it may be described as a lymphoma rash, even though the appearance can be subtle at first.
Distribution matters: lesions often occur on “sun-protected” areas such as the buttocks, hips, lower trunk, or inner thighs. Many patients search online for mycosis fungoides photos to compare patterns, but images can be misleading because the condition varies widely by skin tone, stage, and whether treatments have been used.
Mycosis fungoides can also overlap with everyday skin issues in women such as contact dermatitis from fragrances, hormonal dryness, or irritation from shaving and occlusive clothing. That overlap is exactly why persistent, unexplained patches are usually evaluated with repeat exams and targeted testing rather than appearance alone.
Staging Basics And What Stage 1A Often Means
Staging is based on skin involvement (T), lymph nodes (N), blood (B), and internal organs (M). In mycosis fungoides stage 1a, the skin findings are limited patches or plaques covering less than ten percent of the body surface area, with no significant node, blood, or organ involvement. Many people with early-stage disease live for years with careful monitoring and skin-directed therapy.
How Doctors Confirm The Diagnosis
Diagnosis usually starts with one or more skin biopsies. Pathology may show epidermotropism (T-cells moving into the epidermis) and atypical lymphocytes, but early biopsies can be nonspecific, so repeat biopsies from untreated areas are sometimes needed.
Blood tests can add important context, especially when CTCL is suspected beyond the skin. Flow cytometry in CTCL looks for abnormal T-cell populations in the bloodstream. When clinicians refer to mycosis fungoides flow cytometry, they typically mean measuring markers such as CD3, CD4, CD7, and CD26 to detect an atypical phenotype or quantify circulating malignant cells. T-cell receptor gene rearrangement testing may also be used to look for clonality.
Available Treatments: Skin-Directed And Systemic Options
Mycosis fungoides treatments are chosen based on stage, symptoms, pace of change, and patient goals. Early disease often focuses on controlling inflammation, itch, and visible lesions while limiting long-term side effects.
- Topical therapies: high-potency topical corticosteroids, topical retinoids such as bexarotene gel, and topical chemotherapy like mechlorethamine gel can reduce patches and plaques.
- Phototherapy: narrowband UVB is often used for widespread patch disease; PUVA (psoralen plus UVA) may be used for thicker plaques when appropriate monitoring is available.
- Radiation: localized radiation can treat stubborn plaques or tumors; total skin electron beam therapy is a specialized option for more extensive skin involvement.
- Systemic treatments: interferon-alpha, oral bexarotene, methotrexate, and targeted/biologic options such as brentuximab vedotin or mogamulizumab may be considered in more advanced or refractory cases.
What To Know About Remission And Long-Term Outlook
Two common questions are does mycosis fungoides go away and is mycosis fungoides curable. For many people, especially in early stages, treatment can lead to long periods where skin is clear or nearly clear (remission). However, CTCL can be chronic and relapsing, meaning ongoing follow-up is typical even when symptoms improve.
Tracking symptoms, photographing lesions over time (for personal comparison), and noting what triggers flares can support clearer conversations at follow-ups. Management often includes itch control, gentle skin care, and treatment adjustments rather than a single one-time fix.
FAQs About Signs And Treatment Options
Can Mycosis Fungoides Look Like Eczema Or Psoriasis?
Yes. It can resemble eczema or psoriasis in texture and color, and it may temporarily improve with topical steroids. Persistence, recurrence in the same sites, or unusual distribution can prompt additional biopsies and review by a dermatopathologist.
What Tests Are Common Beyond A Skin Biopsy?
Doctors may use blood work, imaging in selected cases, and immune-cell studies. Flow cytometry and T-cell receptor studies can help characterize CTCL involvement and guide staging, especially if symptoms suggest blood or lymph node involvement.
What Treatments Are Usually Tried First In Early Stage Disease?
Many patients start with skin-directed approaches such as topical steroids, mechlorethamine gel, or phototherapy (often narrowband UVB). Treatment choice depends on lesion thickness, how much skin is involved, and practical considerations like clinic access for light therapy.
When Should Someone Seek Specialist Evaluation?
If a rash persists for months despite appropriate topical therapy, keeps returning, or has an atypical pattern, a dermatology visit and discussion about repeat biopsies and CTCL-focused testing may be appropriate. Some cases benefit from evaluation at centers experienced in cutaneous lymphoma.
Conclusion
Mycosis fungoides is a rare skin lymphoma that can mimic common rashes, especially early on. Recognizing the typical patterns, understanding how diagnosis is confirmed (including biopsy and flow cytometry when needed), and knowing the range of available treatments can make next steps feel more manageable and less mysterious.
Disclaimer: The information provided in this article is for educational and informational purposes only. It does not constitute professional advice. Readers should conduct their own research and consult with qualified professionals before making any decisions.